Dual diagnosis refers to the presence of both a mental health condition and a substance use disorder at the same time, often requiring an integrated approach to care. Clinical patterns tied to co-occurring mental health and substance use disorders show how symptoms from each condition can influence the other and make recovery more complex.
Treating only one condition while ignoring the other can lead to relapse or ongoing instability. Mental health symptoms such as anxiety, depression, or trauma may drive substance use, while substance use can intensify those same symptoms over time. This cycle makes it difficult to achieve lasting progress without a coordinated treatment plan that addresses both sides together.
For individuals seeking structured, comprehensive care, starting dual diagnosis treatment in New Jersey can be an important first step toward stabilization and long-term recovery.

How Do You Know if Dual Diagnosis Treatment in New Jersey is Needed?
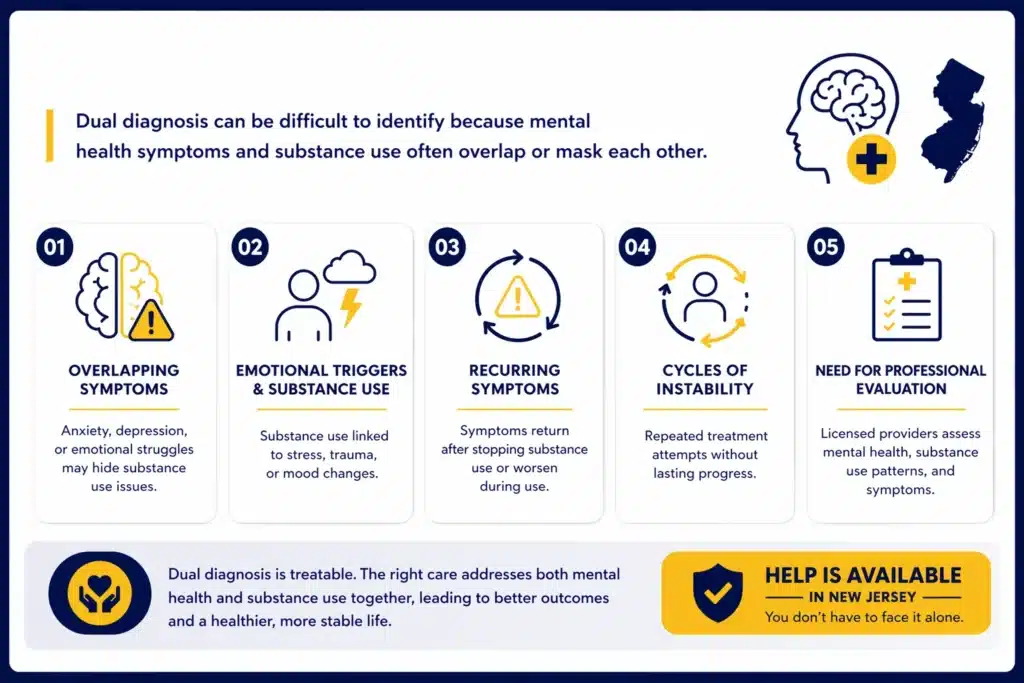
It is not always obvious when both a mental health condition and substance use are present at the same time. In many cases, the symptoms overlap or mask each other. Someone may seek help for anxiety or depression without recognizing how substance use is affecting those symptoms, or they may focus on substance use without addressing underlying emotional or psychological concerns.
There are a few common signs that both conditions may need to be addressed together. These include ongoing mood changes, difficulty managing stress, or patterns of substance use that seem tied to emotional triggers. Some individuals notice that their symptoms return quickly after stopping substance use, while others find that their mental health worsens during periods of use.
Another indicator is difficulty maintaining stability. This can look like repeated attempts at treatment that do not lead to lasting improvement, or cycles of progress followed by setbacks. When both conditions are present, treating only one side often leads to incomplete results.
A full evaluation by a licensed provider is usually the most reliable way to determine what is going on. This process looks at mental health history, substance use patterns, and current symptoms to guide the next steps in care.
What Happens During the Intake Process?
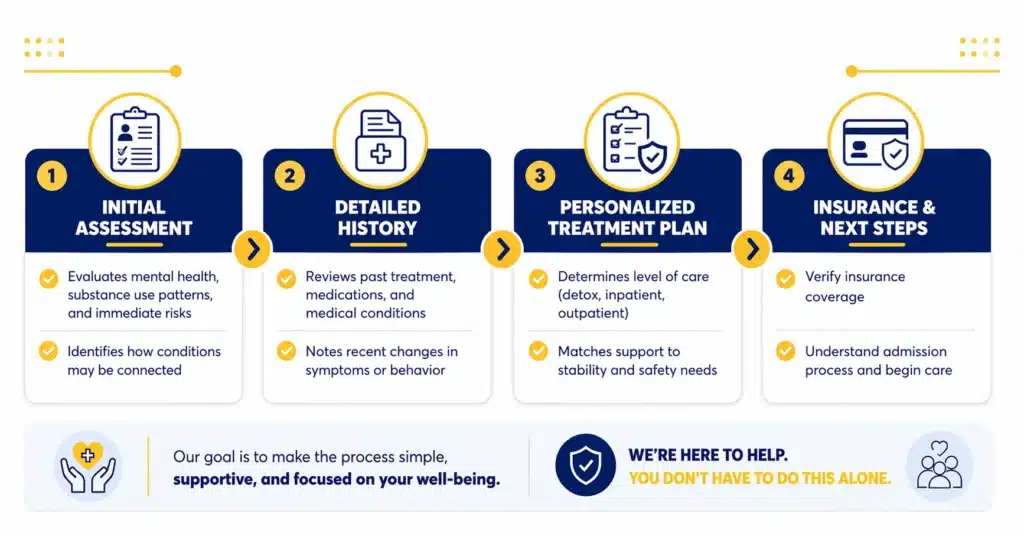
The intake process is designed to gather a clear picture of your current situation so the care team can recommend the right starting point. It usually begins with an initial assessment that covers mental health concerns, substance use patterns, and any immediate risks that need attention. This step helps identify how the two conditions may be connected and what level of support is appropriate.
A detailed history is also part of the intake. This includes past treatment experiences, current medications, medical conditions, and any recent changes in symptoms or behavior. Being open during this stage is important, since accurate information helps shape a plan that reflects your actual needs rather than a general approach.
Once the information is reviewed, the team determines the level of care and outlines a treatment plan. This may include recommendations for detox, inpatient care, or a structured outpatient program, depending on stability and safety. As part of the admissions process, you can also verify your insurance to understand coverage and next steps before starting care.
What Does a Typical Day Look Like in Early Treatment?
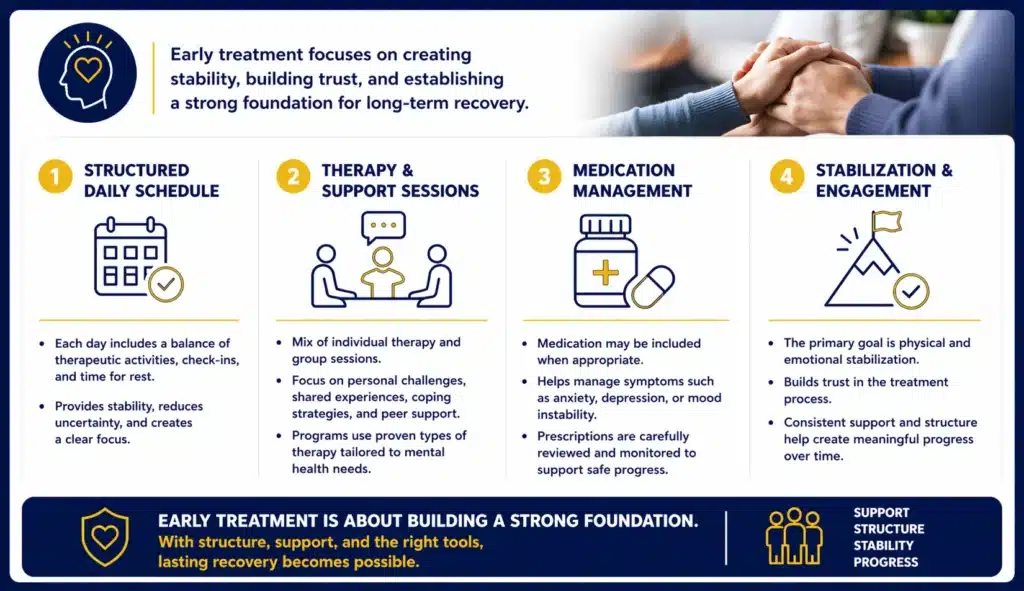
Early treatment usually follows a structured schedule designed to create stability and consistency. Each day is planned to balance therapeutic activities, check-ins, and time for rest. This structure helps reduce uncertainty and gives individuals a clear focus as they adjust to a new environment.
A typical day often includes a mix of individual therapy and group sessions. Individual therapy provides time to address personal challenges, while group sessions focus on shared experiences, coping strategies, and peer support. Many programs use established approaches tailored to mental health needs, including different types of therapy used in mental health treatment.
Medication may be part of the plan when appropriate, especially for managing symptoms such as anxiety, depression, or mood instability. Any prescriptions are carefully reviewed and monitored to ensure they support overall progress without creating additional complications.
In the early stages, the primary goal is stabilization and engagement. This means helping individuals feel physically and emotionally steady enough to participate in treatment while building trust in the process. Over time, the structure and support of a daily routine can make it easier to stay focused and begin making meaningful progress.
What Should Be in Place Before Starting Care?
Preparing for treatment, especially when entering a structured setting like inpatient rehab in New Jersey, involves a few practical steps that can make the transition smoother. This may include arranging time away from work or school, handling financial responsibilities, and making sure any immediate obligations are covered. Taking care of these details in advance can reduce distractions and allow for a more focused start.
Transportation is another important consideration. Knowing how you will get to the facility and return home after treatment helps avoid last-minute complications. It can also be helpful to identify a support system, whether that includes family members, friends, or others who can provide encouragement and stability during this time.
Mental readiness also plays a role. Starting treatment often comes with uncertainty, but having a basic understanding of what to expect can make the process more manageable. Being open to participation, following the program’s structure, and allowing time for adjustment can all support a more productive experience.

Starting Dual Diagnosis Treatment in New Jersey
Starting treatment for both mental health and substance use involves more than choosing a program. It requires a clear understanding of how care works, what to expect during each stage, and how different services fit together. Taking the time to prepare can make the process feel more manageable and reduce uncertainty at the beginning.
Addressing both conditions together gives individuals a better chance at long-term stability. When care is coordinated, it becomes easier to manage symptoms, build healthier patterns, and stay engaged in treatment over time. For those considering treatment, having the right information can make it easier to take the next step and begin care with a stronger sense of direction.
Frequently Asked Questions
What is Dual Diagnosis in Simple Terms?
Dual diagnosis refers to the presence of both a mental health condition and a substance use disorder at the same time. Instead of existing in isolation, these challenges often interact and influence one another, making them more difficult to recognize and address without a more integrated approach.
How Do I Know if it’s More Than Just Stress or Substance Use?
It often comes down to patterns rather than isolated experiences. Ongoing mood changes, repeated reliance on substances to cope, and cycles of temporary relief followed by the return of the same feelings can all suggest something more complex. When these patterns are consistent over time, it may indicate that both mental health and substance use are playing a role.
Can Someone Have a Dual Diagnosis Without Realizing It?
Yes, and it is more common than many people expect. Because the symptoms tend to overlap, it is easy to interpret them as separate or unrelated issues. One side may be more visible, while the other remains less obvious, which can delay recognition.
Why Do Mental Health Issues and Addiction Happen Together?
Mental health challenges and substance use are often connected through coping patterns. Substances may be used to manage stress, anxiety, or low mood, which can provide temporary relief. Over time, this can create a cycle where both the emotional challenges and the substance use continue to influence each other.
Author
-
View all posts
Our editorial team includes licensed clinicians and board-certified addiction specialists. Every article is written and reviewed to be clear, accurate, and rooted in real treatment experience.
-
View all posts
Dr. Williams has held senior leadership positions in the behavioral health field for over 30 years. He has worked with diverse populations in various private and public sectors.












