A dual diagnosis refers to the presence of both a substance use disorder and a co-occurring mental health condition, such as anxiety, depression, or bipolar disorder. These conditions often interact in complex ways, with each influencing symptom severity and overall stability. Because of this connection, care must address both conditions at the same time.
Integrated treatment plays a central role after a dual diagnosis is identified. Focusing on only one condition can leave underlying factors unresolved, increasing the risk of continued symptoms or relapse. A structured approach ensures that mental health and substance use concerns are evaluated together and addressed through coordinated care.
Understanding the next steps after diagnosis helps establish a clear path forward. From assessment and stabilization to ongoing therapy and recovery planning, each phase supports safety, symptom management, and long-term stability.
Understanding a Dual Diagnosis and What It Means for Treatment
Co-occurring disorders, as defined in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR), involve the simultaneous presence of a mental health condition and a substance use disorder. These conditions often influence one another. Substance use may worsen mental health symptoms, while untreated mental health conditions may contribute to continued substance use.
Because of this interaction, treatment must be coordinated. Addressing each condition separately can lead to gaps in care and inconsistent progress. Integrated treatment focuses on both conditions at the same time, using a unified clinical approach.
Care planning for dual diagnosis differs from single-diagnosis treatment by incorporating multiple factors into one structured plan. Mental health symptoms, substance use patterns, and risk factors are evaluated together to guide decisions and ensure continuity throughout treatment.
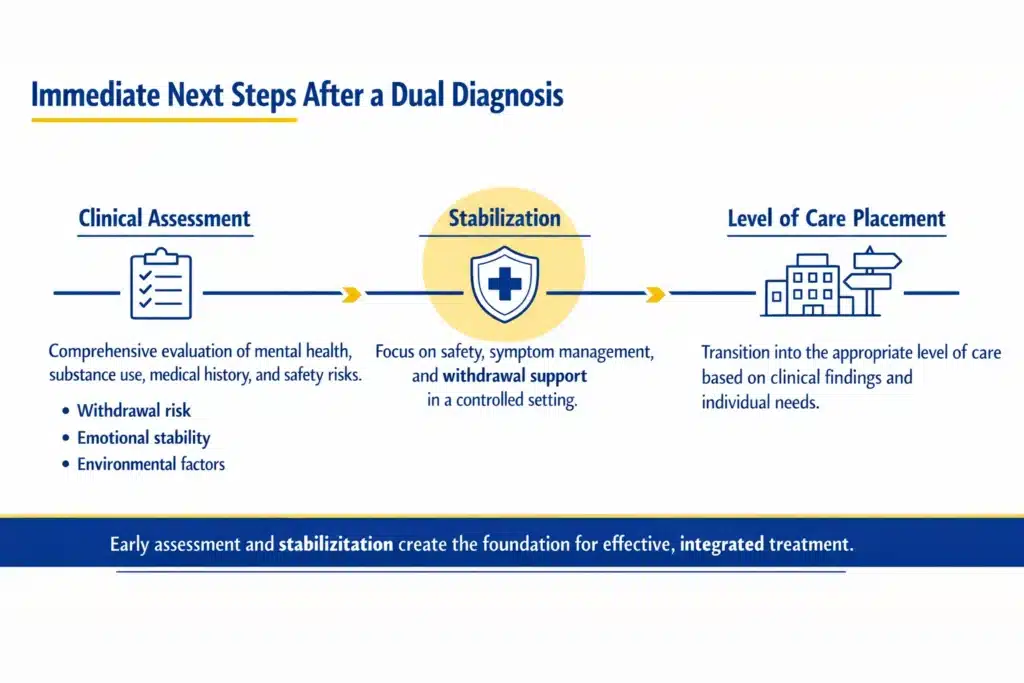
Immediate Next Steps After a Dual Diagnosis
After a dual diagnosis is identified, a comprehensive clinical assessment is typically completed. This process reviews mental health symptoms, substance use history, medical background, and potential safety concerns. Identifying withdrawal risk, emotional stability, and environmental factors helps determine immediate priorities.
Stabilization is often the first focus. This may include addressing withdrawal risk, managing acute mental health symptoms, and ensuring a safe and supportive setting. When necessary, individuals may be referred to appropriate medically supervised settings for short-term stabilization and monitoring.
Following stabilization, the next step involves coordination into an appropriate level of care. This decision is based on clinical findings to ensure that both conditions are addressed within a structured and supportive environment.
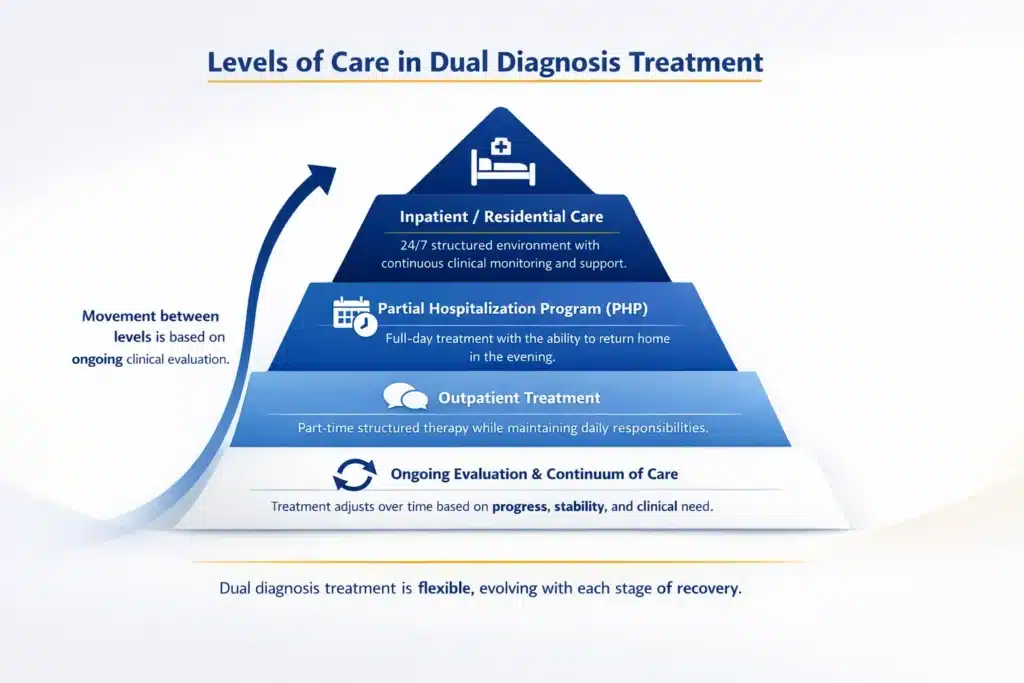
Levels of Care in Dual Diagnosis Treatment
Dual diagnosis care is delivered across several levels, each designed to match clinical needs and overall stability. Movement between levels is based on ongoing evaluation rather than a fixed timeline.
Treatment may begin in a highly structured setting for individuals who require close monitoring and support. Inpatient or residential programs provide a live-in environment with continuous clinical oversight.
Partial hospitalization programs offer intensive, full-day treatment while allowing individuals to return to a stable setting in the evening.
Outpatient care provides structured therapy on a part-time basis. This option supports individuals who are able to maintain daily responsibilities while continuing treatment through structured drug abuse treatment programs.
Each level functions as part of a continuum, allowing care to adjust over time based on progress and clinical need.
How Treatment Plans Are Developed for Co-Occurring Disorders
Treatment plans for dual diagnosis are based on individual clinical needs. A comprehensive evaluation guides the development of a structured plan that addresses both mental health and substance use factors.
Evidence-based approaches are used to support symptom management and behavioral change. These methods are selected based on clinical presentation and are often combined to ensure both conditions are addressed in a coordinated way.
Medication may be included when appropriate to help stabilize certain mental health symptoms or support recovery from substance use. Any use of medication is monitored and adjusted as needed.
Regular clinical review is an ongoing part of the process. As symptoms change or progress is observed, adjustments are made to maintain alignment with current needs. Treatment planning may also take into account factors such as past treatment history, response to previous interventions, and the presence of environmental stressors. These variables can influence both the structure of care and the types of therapeutic approaches used throughout treatment.
Therapy may also address co-occurring conditions through structured interventions that focus on both symptom reduction and long-term behavioral change.
The Role of Therapy in the Dual Diagnosis Recovery Process
Therapy is a central component of dual diagnosis care and is often integrated into structured dual diagnosis treatment programs. Individual therapy provides a structured space to explore patterns related to both mental health and substance use. It also supports the development of practical coping strategies.
Group therapy introduces shared experiences and peer interaction. This setting can help reinforce communication skills and provide additional perspective during recovery. Behavioral approaches like cognitive behavioral therapy and dialectical behavior therapy are commonly used. These methods focus on identifying thought patterns, improving emotional regulation, and building effective responses to stress.
Relapse prevention is integrated throughout therapy. Recognizing triggers and developing structured strategies helps support ongoing stability.
Transitioning From Treatment to Long-Term Recovery
As stability improves, care often shifts to less intensive levels. This transition supports continued progress while allowing for increased independence. Maintaining consistency during this phase is important for reducing disruption in care.
Structured outpatient care plays an important role during this phase. Programs such as Intensive outpatient programs in New Jersey may be part of continued care as individuals transition to more independent routines. Ongoing engagement with structured dual-diagnosis care options can provide continued support as individuals move through different phases of recovery.
Understanding Dual Diagnosis Care Options in New Jersey
Evaluating dual diagnosis care involves understanding how programs are structured and what types of services are available. Licensed and accredited programs follow established clinical standards, which help ensure consistency and safety in care.
Integrated care models are designed to address both mental health and substance use within the same setting. This approach supports continuity and reduces gaps between services. Resources such as the New Jersey treatment provider directory can be used to review available services and better understand how care is organized across the state.
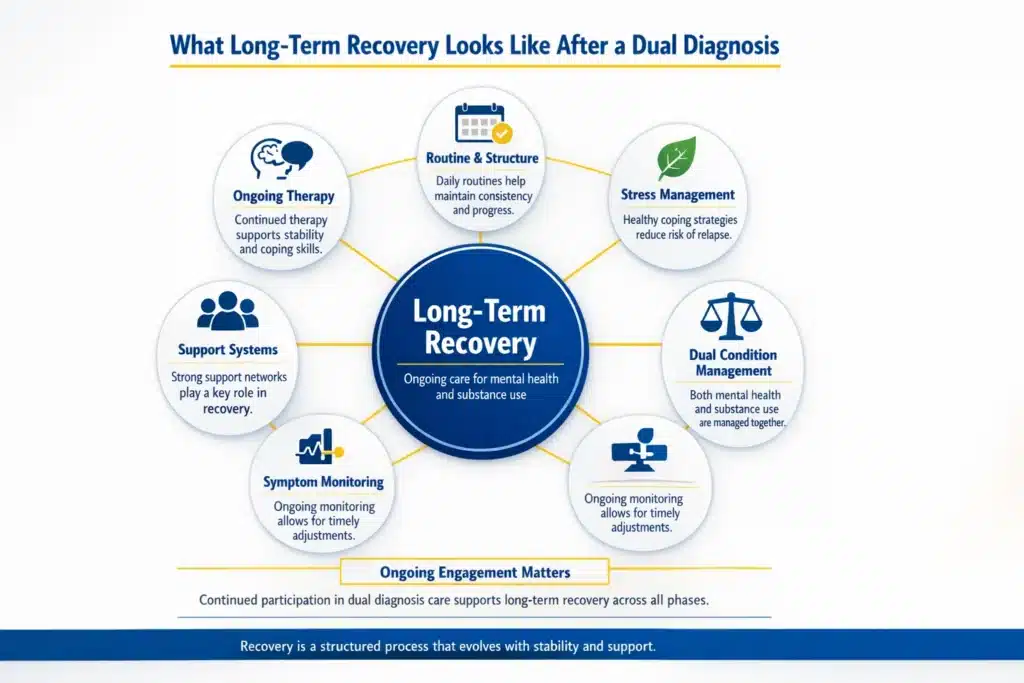
What Long-Term Recovery Looks Like After a Dual Diagnosis
Long-term recovery involves ongoing attention to both mental health and substance use. Continued participation in therapy supports stability and helps reinforce coping strategies over time. Daily structure, stress management techniques, and consistent routines contribute to maintaining progress. Support systems remain an important part of this process.
Monitoring symptoms on an ongoing basis allows for adjustments when needed. Managing both conditions as part of a long-term approach supports continued stability.
Dual Diagnosis Treatment and Long-Term Recovery Outcomes
Long-term recovery following a dual diagnosis depends on consistent management of both mental health conditions and substance use disorders. Integrated treatment remains a central component of this process, supporting stability by addressing co-occurring conditions within a single, coordinated care plan.
Ongoing therapy, structured support, and relapse prevention strategies contribute to maintaining progress over time. As individuals transition between levels of care, continuity and clinical oversight help reduce the risk of symptom recurrence and support sustained stability.
Treatment outcomes are influenced by several factors, including the severity of each condition, engagement in care, and access to appropriate clinical resources. Programs that provide coordinated services across multiple levels of care can support more consistent outcomes by adapting to changing needs throughout the recovery process.
Access to structured care, including evidence-based approaches, plays a role in supporting long-term stability and continued progress following diagnosis.
Frequently Asked Questions About Dual Diagnosis Treatment
What Happens After a Dual Diagnosis is Made?
A clinical assessment is completed to evaluate symptoms, risks, and care needs. Initial steps often focus on stabilization, followed by placement into an appropriate level of care and ongoing therapy.
How Long Does Dual Diagnosis Treatment Last?
The length of treatment varies based on individual needs and symptom severity. Care may include multiple stages, from early stabilization to continued outpatient support.
Is Detox Always Required for Dual Diagnosis Treatment?
Detox is only necessary when there is a risk of withdrawal from substances. It is not required in all cases, but may be recommended when physical dependence is present.
Can Mental Health and Substance Use Disorders Be Treated at the Same Time?
Yes, integrated treatment is designed to address both conditions simultaneously. This approach supports more consistent symptom management and long-term stability.
Author
-
View all posts
Our editorial team includes licensed clinicians and board-certified addiction specialists. Every article is written and reviewed to be clear, accurate, and rooted in real treatment experience.
-
View all posts
Dr. Williams has held senior leadership positions in the behavioral health field for over 30 years. He has worked with diverse populations in various private and public sectors.












