Alcohol withdrawal is a potentially serious medical condition that occurs when someone with alcohol dependence suddenly stops or significantly reduces drinking. In some cases, symptoms progress beyond mild discomfort and develop into severe complications affecting the brain and cardiovascular system.
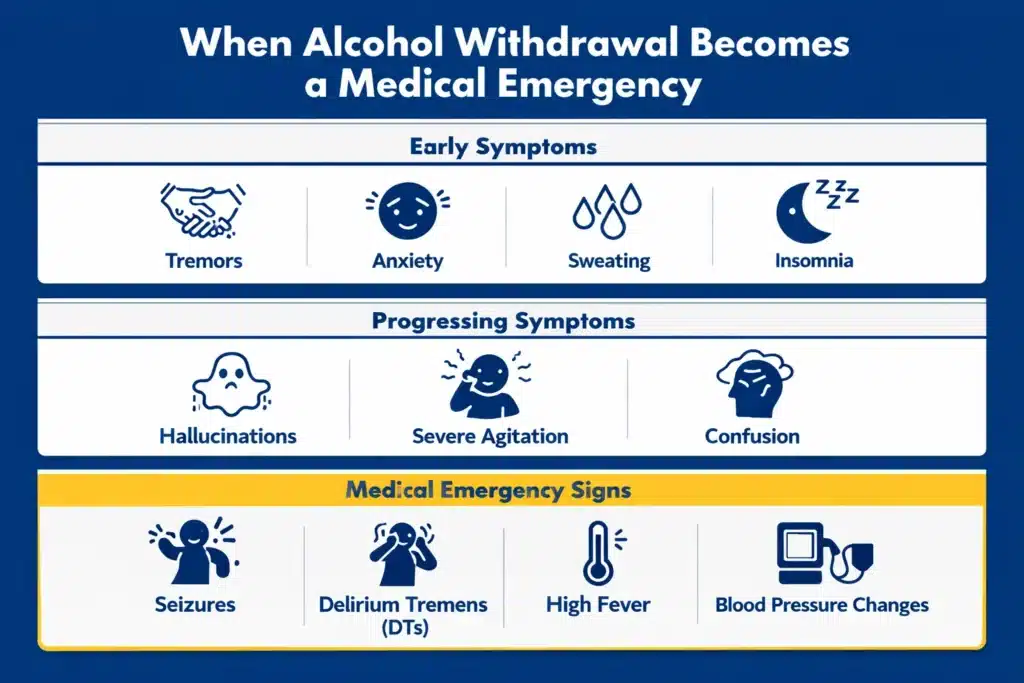
Early symptoms often begin within hours and may include tremors, anxiety, sweating, and insomnia. As withdrawal progresses, more dangerous symptoms can emerge, including seizures, hallucinations, and delirium tremens (DTs), a life-threatening condition marked by confusion, fever, and severe agitation. A clinical review in The New England Journal of Medicine identifies severe alcohol withdrawal as a condition associated with seizures, delirium tremens, and cardiovascular instability.
Because symptoms can escalate quickly, recognizing when alcohol withdrawal becomes a medical emergency is essential. Severe cases require immediate medical evaluation and continuous monitoring to reduce the risk of life-threatening complications.
Understanding Alcohol Withdrawal and Physical Dependence
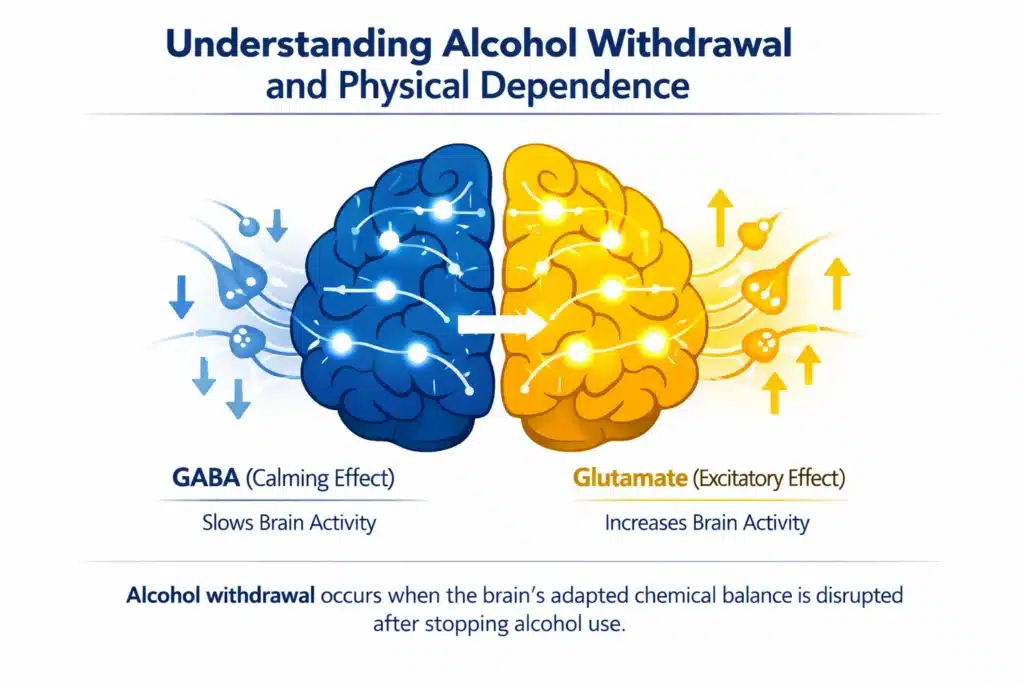
Alcohol withdrawal develops due to long-term changes in brain chemistry caused by repeated alcohol use. Alcohol slows brain activity by enhancing gamma-aminobutyric acid (GABA) and suppressing glutamate, which stimulates nerve signaling. Over time, the brain adapts by reducing sensitivity to GABA and increasing glutamate activity to maintain balance.
When alcohol use suddenly stops, this balance is disrupted. The brain becomes overactive because inhibitory signals no longer counteract heightened excitatory activity, leading to withdrawal symptoms.
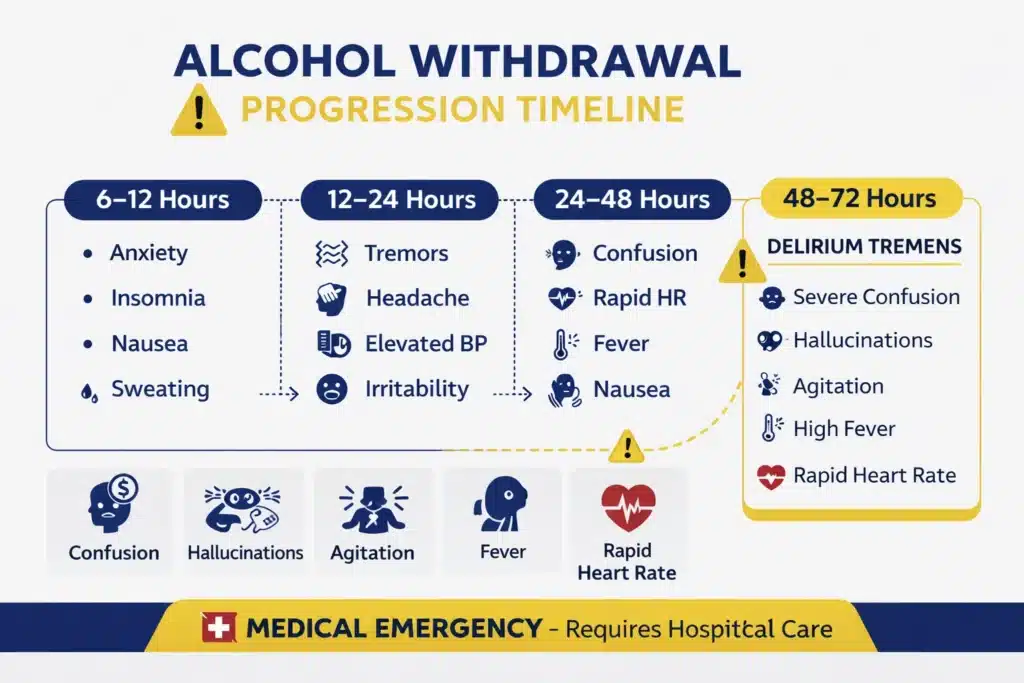
Physical dependence forms as the brain and body adjust to functioning with alcohol present. Once dependence develops, abruptly stopping alcohol use can trigger a range of symptoms as the body attempts to regain stability. Early symptoms typically begin within six to twelve hours after the last drink and may intensify over the following one to three days.
Common Alcohol Withdrawal Symptoms
Alcohol withdrawal produces a range of physical and neurological symptoms that can progress in severity over time.
Mild symptoms often begin within several hours after the last drink and commonly include anxiety, tremors, sweating, nausea, headache, and insomnia. Tremors, particularly in the hands, are among the most recognizable early signs. Restlessness, irritability, and difficulty sleeping are also common during this stage.
As withdrawal progresses, symptoms may intensify into a moderate stage marked by increased heart rate, elevated blood pressure, confusion, and persistent vomiting. These changes indicate greater physiological stress and signal an increased risk of complications.
In individuals with more significant alcohol dependence, symptoms can escalate quickly from mild discomfort to severe neurological or cardiovascular complications, requiring closer medical evaluation.
When Alcohol Withdrawal Becomes a Medical Emergency
Alcohol withdrawal can escalate quickly in individuals with significant physical dependence. What begins as mild symptoms such as tremors, anxiety, nausea, and sweating may progress into serious complications. Severe alcohol withdrawal is considered a medical emergency due to the risk of life-threatening instability.
Certain warning signs require immediate medical attention. Seizures are among the most serious complications and often occur within the first forty-eight hours after the last drink. Hallucinations, severe agitation, and extreme confusion indicate worsening neurological disturbance.
Delirium tremens (DTs), the most severe form of alcohol withdrawal, involves sudden changes in mental status, fever, intense agitation, and severe autonomic dysfunction. High fever, dehydration, and dangerous spikes in blood pressure further signal a critical condition.
These symptoms require urgent medical evaluation and continuous monitoring in a hospital or specialized withdrawal management settings. After medical stabilization, individuals often transition into ongoing evidence-based care such as medication-assisted treatment for alcohol use disorder, which combines FDA-approved medications with behavioral therapy to support long-term recovery.

Delirium Tremens (DTs): The Most Severe Form of Alcohol Withdrawal
Delirium tremens, commonly abbreviated as DTs, represents the most severe and dangerous form of alcohol withdrawal syndrome. This condition develops in individuals with significant alcohol dependence when the brain and nervous system enter a state of extreme hyperactivity after alcohol use stops. Delirium tremens produces sudden disturbances in mental status, severe autonomic instability, and rapidly worsening neurological symptoms.
DTs typically appear between forty-eight and seventy-two hours after the last drink, although symptoms occasionally emerge later in cases of prolonged alcohol dependence. The condition begins with profound confusion and disorientation as the brain struggles to regulate neurotransmitter activity. Individuals experiencing delirium tremens frequently develop vivid visual or auditory hallucinations, severe agitation, and intense anxiety.
Physical symptoms reflect widespread autonomic nervous system activation. High fever, rapid heart rate, elevated blood pressure, and heavy sweating commonly occur as the body enters a state of severe physiological stress.
Untreated delirium tremens carries significant medical risk. Severe dehydration, cardiac complications, and uncontrolled seizures develop without medical intervention. Because of these dangers, delirium tremens requires hospital-level monitoring and immediate medical stabilization.
Risk Factors for Severe Alcohol Withdrawal
Not every individual who stops drinking develops severe alcohol withdrawal. Certain medical histories and patterns of alcohol use significantly increase the risk of dangerous complications during withdrawal. Identifying these risk factors helps determine when closer medical supervision and monitoring become necessary.
Long-term heavy alcohol use represents the strongest predictor of severe withdrawal. Prolonged exposure to alcohol forces the brain and nervous system to adapt to the constant presence of a depressant substance. When alcohol use stops abruptly after years of heavy consumption, the nervous system reacts with intense hyperactivity that increases the risk of seizures, delirium tremens, and cardiovascular instability.
Previous withdrawal episodes also increase the likelihood of severe symptoms. Research describing the kindling effect in alcohol withdrawal explains that repeated withdrawal episodes progressively increase brain excitability. Each subsequent withdrawal period produces more intense neurological symptoms and a greater likelihood of complications.
Additional factors further elevate risk. A history of withdrawal seizures strongly predicts future seizure activity during withdrawal. Co-occurring medical conditions, older age, polysubstance use, and untreated mental health disorders also increase the danger of severe withdrawal symptoms. Individuals with these risk factors require careful medical evaluation when alcohol withdrawal begins because complications develop rapidly without appropriate monitoring.
Medical Supervision and Management of Alcohol Withdrawal
Medical supervision is often necessary during alcohol withdrawal when symptoms move beyond mild discomfort or when risk factors for severe complications are present. Withdrawal can place significant stress on the brain and cardiovascular system, and symptoms may escalate quickly without proper monitoring.
In medically supervised settings, healthcare professionals monitor vital signs, assess symptom progression, and intervene if complications develop. This level of care helps reduce the risk of seizures, severe agitation, and other dangerous effects of withdrawal.
Medications may be used in some cases to stabilize the nervous system, reduce seizure risk, and manage severe symptoms. Supportive care, including hydration and electrolyte balance, also plays an important role in preventing complications.
These services are typically provided in hospital settings or specialized withdrawal management programs, where continuous observation ensures that symptoms are safely managed before transitioning to ongoing addiction treatment, such as inpatient rehab programs that provide structured, supportive care during early recovery.
Emergency and Crisis Withdrawal Care in New Jersey
Severe alcohol withdrawal requires immediate medical attention when symptoms escalate. Hospitals and specialized withdrawal management facilities provide care necessary to stabilize individuals experiencing dangerous complications. These medical environments manage other life-threatening effects associated with severe alcohol withdrawal.
Medical stabilization focuses on controlling withdrawal symptoms while protecting vital organ systems. Healthcare professionals monitor heart rate, blood pressure, body temperature, and neurological status to detect early signs of complications. Continuous observation remains essential because conditions such as seizures, delirium tremens, severe dehydration, and extreme agitation develop rapidly without proper intervention.
Families searching for urgent care for alcohol withdrawal often seek immediate medical support when symptoms become severe. Online searches frequently reference crisis detox services or emergency drug detox in New Jersey, which generally refer to hospital-based withdrawal management or specialized facilities equipped to stabilize individuals experiencing severe withdrawal complications.
Once withdrawal symptoms stabilize and immediate medical risks resolve, individuals often transition into ongoing addiction treatment. Structured treatment programs provide therapy, behavioral support, and recovery planning designed to address alcohol use disorder and reduce relapse risk after withdrawal stabilization.
Treatment and Recovery After Alcohol Withdrawal Stabilization
Stabilization from alcohol withdrawal represents an important first step in addressing alcohol use disorder, but long-term recovery requires ongoing treatment beyond the withdrawal period. Once immediate medical risks resolve, structured addiction treatment helps individuals address the behavioral, psychological, and social factors that contribute to ongoing alcohol use.
Some individuals begin recovery in inpatient addiction treatment settings, where a structured environment provides intensive therapeutic support during the early stages of sobriety. Residential programs often include individual counseling, group therapy, and education designed to help individuals understand substance use patterns and develop healthier coping strategies.
Others continue recovery through outpatient treatment while maintaining responsibilities such as work, school, or family obligations. Understanding the differences between inpatient and outpatient rehab programs helps individuals determine which level of care best supports their recovery needs after alcohol withdrawal stabilization.
Behavioral therapy, relapse prevention planning, and ongoing recovery support remain essential components of treatment. Mental health care also plays an important role in recovery, particularly for individuals experiencing co-occurring conditions such as anxiety, depression, or trauma-related disorders. Integrated treatment that addresses both substance use and mental health concerns supports long-term stability and reduces the likelihood of relapse following alcohol withdrawal.
Alcohol withdrawal ranges from mild discomfort to severe medical emergencies that require immediate attention. Recognizing the warning signs of dangerous withdrawal symptoms helps ensure that individuals experiencing complications receive appropriate medical care. Understanding the risks, symptoms, and treatment pathways associated with alcohol withdrawal provides important context for families and individuals navigating this complex and potentially life-threatening condition.
Frequently Asked Questions About Alcohol Withdrawal Emergencies
How Long Does Alcohol Withdrawal Usually Last?
Symptoms typically begin within six to twelve hours after the last drink. Mild symptoms appear first and may include anxiety, tremors, nausea, and insomnia. Symptoms often peak between twenty-four and seventy-two hours, when severe complications such as seizures or delirium tremens may occur. While many symptoms improve after several days, recovery varies based on overall health and severity of dependence.
Can Alcohol Withdrawal Cause Seizures?
Yes. Seizures are a serious complication of alcohol withdrawal and often occur within the first forty-eight hours after stopping alcohol. Risk is higher in individuals with a history of heavy alcohol use or prior withdrawal episodes.
When Should Alcohol Withdrawal Be Treated in a Hospital?
Hospital care is necessary when severe symptoms or complications are likely. Warning signs include seizures, hallucinations, severe agitation, high fever, confusion, and dangerous changes in heart rate or blood pressure.
What is Delirium Tremens?
Delirium tremens (DTs) is the most severe form of alcohol withdrawal. It typically develops within forty-eight to seventy-two hours and includes confusion, agitation, hallucinations, fever, and rapid heart rate. Without treatment, it can be life-threatening.
Is Medical Supervision Necessary During Alcohol Withdrawal?
Medical supervision is recommended when symptoms go beyond mild discomfort or when risk factors for severe withdrawal are present, such as long-term heavy alcohol use or prior withdrawal complications.
Where Can Emergency Alcohol Withdrawal Treatment Be Found in New Jersey?
Emergency treatment is provided in hospitals and specialized withdrawal management facilities. These settings offer monitoring and stabilization for severe symptoms, followed by transition into ongoing addiction treatment when appropriate.
Author
-
View all posts
Our editorial team includes licensed clinicians and board-certified addiction specialists. Every article is written and reviewed to be clear, accurate, and rooted in real treatment experience.
-
View all posts
Dr. Williams has held senior leadership positions in the behavioral health field for over 30 years. He has worked with diverse populations in various private and public sectors.












